New Microscope Reveals Interactions Between Drugs and Receptors
Trend Watch: Advances in Healthtech Benefit Oncology, Military Docs, Patients, Drug Delivery, and More
Researchers at Case Western Reserve University School of Medicine have used a cryo-electron microscopy technique to observe the interactions between a drug molecule and its protein receptor. The approach provides valuable information, which could offer clues as to how to modify drug molecules to improve their effectiveness.
This new technique is called single-particle cryo-electron microscopy and it involves cooling a sample down to very low temperatures and then imaging it using a new type of electron microscope. The technique allows researchers to image drug/receptor interactions at less than a billionth of one meter.
In the future, the technique could lead to more effective drugs by providing researchers with a wealth of information on drug/target interactions.
The way that drug molecules bind to their target receptors in the body can have significant consequences in terms of their efficacy. Enhancing drug binding could lead to better therapeutic effects for a wider range of patients. To achieve this, researchers need to understand the role of various components of the drug molecule in the interaction with the receptor binding pocket. However, observing and modeling the interactions between drug molecules and their target receptors is challenging.
“In the past, we didn’t have the confidence to model the drug in its binding pocket," says Sandip Basak, a researcher involved in the study. “Now we can precisely do that. We can also watch the drug move in the pocket using molecular dynamics simulations."
The research team used single-particle cryo-electron microscopy to investigate the interaction of setrons, a class of drugs used to manage vomiting and nausea, with their target serotonin receptors in the gastrointestinal tract. Setrons don’t work for everyone, meaning that there is room for improvement. “Cancer patients who have vomiting later in their treatment plans — delayed emesis — don’t tend to respond to setrons," says Sudha Chakrapani, another researcher involved in the study. “There is a constant need for better drugs."
Rutgers: Cancer Device Can Test if Targeted Chemo is Working
Rutgers researchers have created a device that can determine whether targeted chemotherapy drugs are working on individual cancer patients.
The portable device, which uses artificial intelligence and biosensors, is up to 95.9% accurate in counting live cancer cells when they pass through electrodes, according to a study in the journal Microsystems & Nanoengineering.
“We built a portable platform that can predict whether patients will respond positively to targeted cancer therapy," says senior author Mehdi Javanmard, an assistant professor in the Department of Electrical and Computer Engineering in the School of Engineering at Rutgers University–New Brunswick. “Our technology combines artificial intelligence and sophisticated biosensors that handle tiny amounts of fluids to see if cancer cells are sensitive or resistant to chemotherapy drugs."
The device provides immediate results and will allow for more personalized interventions for patients as well as better management and detection of the disease. It can rapidly analyze cells without having to stain them, allowing for further molecular analysis and instantaneous results. Current devices rely on staining, limiting the characterization of cells.
“We envision using this new device as a point-of-care diagnostic tool for assessing patient response and personalization of therapeutics," the study authors say.
The Rutgers team tested the new device using cancer cell samples treated with different concentrations of a targeted anticancer drug. The device detects whether a cell is alive based on the shift in its electrical properties as it passes through a tiny fluidic hole. The next step is to perform tests on tumor samples from patients. The researchers hope the device will be used to test cancer therapies before treatment.
MedCognition Develops AR Patient Simulator System for Military Medical Training
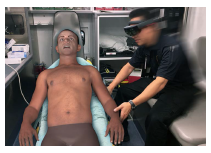 MedCognition, a Texas-based start-up company, is collaborating with Chenega Healthcare Services on a military medicine education and training initiative for the U.S. Army. MedCognition will create military-relevant trauma training modules using its PerSim augmented reality patient simulator system to support tactical combat casualty care and emulate battlefield and mass casualty incident injuries as part of the $750,000 development contract. MedCognition will develop the training modules over the next 12 months with the potential to be adopted by the U.S. military in the years to come.
MedCognition, a Texas-based start-up company, is collaborating with Chenega Healthcare Services on a military medicine education and training initiative for the U.S. Army. MedCognition will create military-relevant trauma training modules using its PerSim augmented reality patient simulator system to support tactical combat casualty care and emulate battlefield and mass casualty incident injuries as part of the $750,000 development contract. MedCognition will develop the training modules over the next 12 months with the potential to be adopted by the U.S. military in the years to come.
The PerSim augmented reality patient simulator system provides dynamic realism in medical simulation training using Microsoft HoloLens Mixed reality to project life-like holographic patients into actual work environments. PerSim allows participants to view realistic patient simulations with a number of clinical presentations, including respiratory distress, stroke and minor trauma, and is currently used by pre-hospital training programs to strengthen critical thinking, decision-making, and assessment skills of trainees.
“Experiential learning is a cornerstone of providing quality patient care and potentially preventing medical errors, especially in a frantic and stressful environment like pre-hospital," says U.S. Army Combat Veteran Physician and CEO of MedCognition, Dr. Kevin King. “MedCognition delivers affordable, realistic, and portable tools for first responders and healthcare clinicians to learn through hands-on experience. Instead of classrooms or on-screen training modules, PerSim empowers educators and trainees to practice caring for critically ill patients with the tools and in the actual environments where they deliver care. This contract expands our capabilities into military medicine and battlefield care, with the hope that this could help save the lives of critically ill and injured soldiers."
MIT: Nanoemulsion Gels Offer New Way To Deliver Drugs Through Skin
 In research sponsored by the personal care company L’Oréal, MIT chemical engineers found a way to create very tiny droplets of one liquid suspended within another liquid, known as nanoemulsions.
In research sponsored by the personal care company L’Oréal, MIT chemical engineers found a way to create very tiny droplets of one liquid suspended within another liquid, known as nanoemulsions.
The researchers also found a way to easily convert the liquid nanoemulsions to a gel when they reach body temperature, which could be useful for developing materials that can deliver medication when rubbed on the skin or injected into the body.
“The pharmaceutical industry is hugely interested in nanoemulsions as a way of delivering small molecule therapeutics," says Patrick Doyle, the Robert T. Haslam professor of chemical engineering and the senior author of the study. “This could be topically, through ingestion, or by spraying into the nose, because once the size range reaches hundreds of nanometers permeation in the skin is much more effective."
Professor Doyle is now exploring ways to incorporate a variety of active pharmaceutical ingredients into this type of gel. Such products could be useful for delivering topical medications to help heal burns or other types of injuries or could be injected to form a “drug depot" that would solidify inside the body and release drugs over an extended period of time. These droplets could also be made small enough that they could be used in nasal sprays for delivering inhalable drugs, Professor Doyle says.
In a new study, which appeared in the June 21 issue of Nature Communications, the researchers created nanoemulsions that were stable for more than a year. To demonstrate the emulsions’ potential usefulness for delivering drugs, the researchers showed that they could incorporate ibuprofen into the droplets.
Nanoemulsions, which contain droplets with a diameter 200 nanometers or smaller, are desirable not only because they are more stable, but they also have a higher ratio of surface area to volume, which allows them to carry larger payloads of active ingredients such as drugs or sunscreens.
OpenMD.com Lists Top 750 Health Websites
 The Internet provides instant access to vast amounts of medical information. However, separating credible from questionable sources remains a challenge. OpenMD.com has built a health site directory to help users locate trustworthy sources of free medical information.
The Internet provides instant access to vast amounts of medical information. However, separating credible from questionable sources remains a challenge. OpenMD.com has built a health site directory to help users locate trustworthy sources of free medical information.
The directory indexes more than 750 freely accessible sources of medical information. Sites are organized across more than 30 categories, including health tools (symptom checkers, pill identifiers, etc.), news, student resources, and medical specialties.
All sites are reviewed for content quality, accessibility, credibility, and usability. Among those sites, only the best are included. The directory is maintained with the regular input of medical professionals.
OpenMD also developed several research guides aimed at helping users evaluate the credibility of sources and make use of the medical information they find online.
Launched earlier this year, OpenMD.com is a health search engine that provides access to billions of documents from global health organizations, medical journals, health publishers, and government agencies. The engine prioritizes content from free and open access sources.
Anthem, K Health Team up on Personalized Primary Care Tool for Members
Anthem and K Health, a consumer-focused digital health company, are partnering to develop a new app that seeks to help patients get personalized information and connect to doctors.
The partners are creating a co-branded app tool that will allow Anthem members to chat with a doctor for “less than a copay." Additionally, members will now have access to K Health’s existing tool, which gives users insights into how doctors have diagnosed patients with similar symptoms in the past.
While the amount is not specified, according to material provided by K Health, Anthem is also making an investment of “tens of millions of dollars" to the startup to help with the development of this tool.
Increasingly, payers are looking for alternative ways to facilitate care. In a similar vein, telehealth company Doctor on Demand and Humana jointly launched a new virtual care model that would allow plan members to access in-network primary care doctors with no copay.
The co-branded application will open up access to K Health’s AI-driven triage and symptom checker tool to Anthem’s more than 40 million members. Using a combination of licensed data resources and a chatbot-driven patient interview about demographics, medical history and symptoms, K Health’s system is able to derive likely conditions based on other similar patient cases and recommend potential routes to receive care.
K Health’s application was launched in the U.S. last year and has grown to more than 1.3 million users. The company hopes the new Anthem partnership will enable the company to reach 10 million users by the end of 2020.
Anthem members will be able to receive symptom checker services for free and connect with a board-certified doctor through the app. While the pricing is still being worked out for the co-branded Anthem service, K Health’s standard application has a $49 annual fee for unlimited chat messages with a doctor.
The doctor will help discuss treatment options through chat and have the ability to prescribe medication or lab tests if necessary. K Health has a roster of around 50 clinicians employed by an associated physicians group and currently offers services in 14 states between the hours of 11 a.m. and 11 p.m.
K Health touts its technology as being more personalized and accurate than simple internet searches or more generalized symptom checkers, while also being able to close the loop of care and directly connect patients to clinicians. (PV)