It is 2022 – welcome to a new era of healthcare, where patients are No. 1.
It is 2022 – welcome to a new era of healthcare, where patients are No. 1.
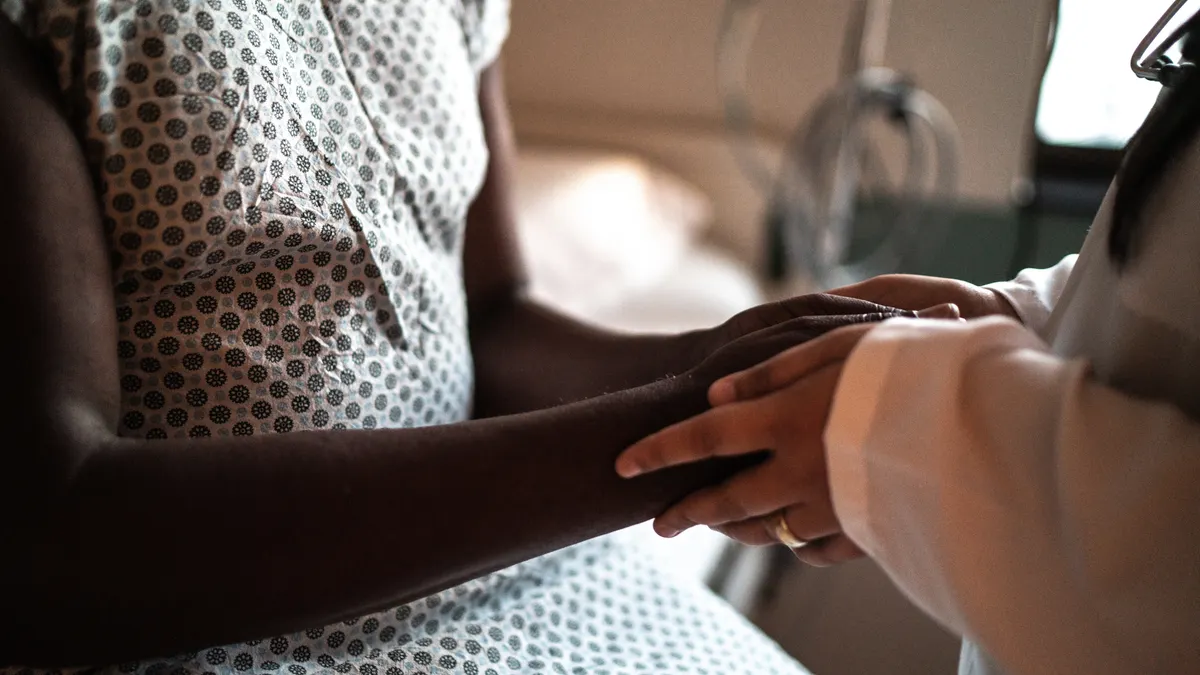
With this phrasing, you may envision a football game of healthcare with rowdy fans waving foam fingers in the air, chanting boisterous incantations of support for Team Patient. Of course, this is not a game but rather the result of a multi-year shift, suddenly accelerated by the COVID-19 pandemic of 2020.
In this new healthcare arena, patients inform clinical trial protocol design, clinician visits, and evidence capture methodology. The decentralized clinical trial (DCT) model embraced by stakeholders in high numbers from the start of the pandemic through to today has empowered truly patient-centric drug development. And, in doing so, it has democratized access to medical research for the emergence of a global ecosystem that truly enables research anytime, anywhere, and for every person.
DCT Platforms Remove Bottlenecks
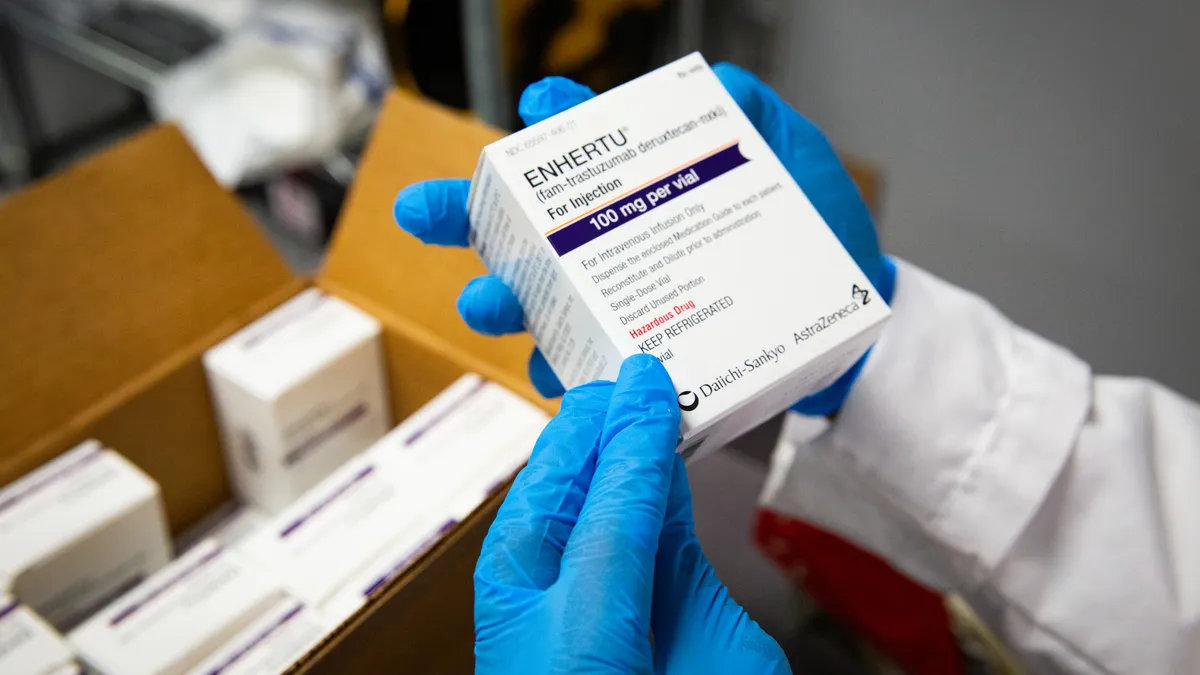
 DCT platforms now provide remote access to new investigational medicines to patients worldwide by removing traditional bottlenecks and streamlining key processes. By design, DCTs provide freedom to create trial designs that work best for each site, each protocol, and each patient. They allow patients to have physician-monitored access to potentially life-altering new therapies from their homes. And, because patients’ health is surveilled continuously with wearables, electronic diaries, virtual check-ins, and other tools, they receive premier care.
DCT platforms now provide remote access to new investigational medicines to patients worldwide by removing traditional bottlenecks and streamlining key processes. By design, DCTs provide freedom to create trial designs that work best for each site, each protocol, and each patient. They allow patients to have physician-monitored access to potentially life-altering new therapies from their homes. And, because patients’ health is surveilled continuously with wearables, electronic diaries, virtual check-ins, and other tools, they receive premier care.
Greater Patient-Centric Care
Real-world data from “in-the-moment" patient accounts — before memory-muddled experiences are recanted at the next in-person visit weeks later — improve data quality and drive better outcomes. The more we understand about patients in the context of their home environments and day-to-day lives, companies can continuously improve the design of digital solutions for greater patient-centric care.
For instance, an asthmatic patient who is enrolled in a clinical trial must commute to and from work via public transit. If doctors can see that the oxygen levels for the patient are impacted by the outdoor environment and that this exacerbates their disease rather than the experimental therapy, then treatment may include different travel arrangements rather than a change in dosage. The expansion of digital data to characterize symptoms, endpoints, and treatment efficacy further personalizes and improves patient outcomes.
Machine Learning Leads to Better Data Usage
 Electronic diaries, wearable information, ECG monitors, and other measurements can be overlaid with, say, geolocation data to build a detailed, multi-layered profile of the patient with real-world context. We are applying machine learning to understand how to best use this data to detect disease state, symptom triggers, prevalence, and disease progression. In fact, researchers are now able to capture quality data remotely, on a longitudinal scale, and harness that data across groups of patients to establish accurate digital biomarkers.
Electronic diaries, wearable information, ECG monitors, and other measurements can be overlaid with, say, geolocation data to build a detailed, multi-layered profile of the patient with real-world context. We are applying machine learning to understand how to best use this data to detect disease state, symptom triggers, prevalence, and disease progression. In fact, researchers are now able to capture quality data remotely, on a longitudinal scale, and harness that data across groups of patients to establish accurate digital biomarkers.
A daily video that shows progressive changes to a Parkinson’s patient’s shuffle, for example, or a wearable device that measures hand tremors continuously, or a digital sleep monitor that tracks REM sleep cycles all inject new factors into the research equation to help determine accurate digital signatures. As a result, science can identify the early “simmering" symptoms that could turn into an adverse event. Since the development of symptoms has the potential to jeopardize patient safety and instill fear and panic – patients could drop out of a trial prematurely. Identify these early, however, and there’s a chance to mitigate symptoms, prevent psychological harm, and avoid losing participation.
Increase Access to Treat More Diverse Populations
With increased trial access and greater trial retention across all demographics, too, study data is now more all-encompassing for greater insight into developing new treatments that help more people. Medable customers achieved unprecedented results in 2020 with three-times faster enrollment and more than 90% retention rates.
Indeed, the decentralized model has opened doors to more patients and reduced racial disparity in healthcare to improve overall outcomes. For decades, there was tacit acknowledgement of a two-tier healthcare system in the United States — 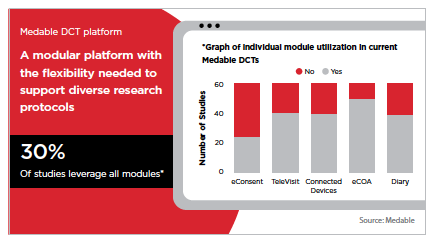 those who had access to quality healthcare and those who did not. The difference between the two tipped the scales of population representation in trials, an issue that caused significant health risks, as diverse patient populations have different responses to certain diseases and pharmaceuticals.
those who had access to quality healthcare and those who did not. The difference between the two tipped the scales of population representation in trials, an issue that caused significant health risks, as diverse patient populations have different responses to certain diseases and pharmaceuticals.
Moderna and Pfizer’s COVID-19 vaccine trials faced scrutiny for trial participants not adequately representing the general population and those most impacted by COVID-19, for instance.1 The FDA expanded its guidelines2 for enhancing the diversity of clinical trial populations. However, nothing has done more to improve diversity than the decentralization of trials. DCTs bring the trial to the patient, removing the burdens of travel and distance, and the need to take time off from work, to make trials feasible across demographics.
Modular Flexibility
To succeed with this new model, look for a platform that provides modular flexibility, so patients have options. Most life-sciences companies combine different modules — i.e., televisit, e-consent, and connected devices — together in a decentralized environment to enable a personalized experience for patients. In fact, 30% of all Medable clients that initiated decentralized studies in 2020 used all the modules together on a unified platform for greater visibility, connectivity, and a single record of truth.
What started as the industry’s effort to remedy a pandemic emergency in 2020 and optimize clinical trial execution blossomed into something much more transformative. The decentralized model gave birth to a new healthcare environment, where digital enablement empowers patient choice. If 2020 was the match, 2021 was the fuel that enabled the spread of a new model for a new era of patient care today.
Notes:
1 https://www.fastcompany.com/90555722/why-covid-19-vaccine-trials-still-need-more-diversity
2 https://www.fda.gov/media/127712/download
Medable offers the most flexible decentralized clinical trial platform — helping streamline clinical trials for patients, research sites, and clinicians whether in-clinic or at home. Medable’s completely modular approach allows pharmaceutical companies and clinical research organizations (CROs) to use what they want, not what they don’t — scaling up and down hybrid research capabilities to better suit their unique studies. Founded by a clinician and led by seasoned clinical trial operational and science expertise, Medable is trusted by five of the top 10 pharmaceutical companies and five of the top seven CROs.
For more information, visit medable.com and follow @Medableinc onTwitter.