The world and technology are racing ahead of the clinical trials industry. Digital health technologies (DHTs) continue to advance while clinical research remains slow to embrace efficient technologies and offerings that are widely being deployed in healthcare. The result is a market where a new medical product costs in excess of $2 billion and takes over 10 years to get to market — if it even makes it to market.
The world and technology are racing ahead of the clinical trials industry. Digital health technologies (DHTs) continue to advance while clinical research remains slow to embrace efficient technologies and offerings that are widely being deployed in healthcare. The result is a market where a new medical product costs in excess of $2 billion and takes over 10 years to get to market — if it even makes it to market.
With advanced technologies now a part of our daily lives, clinical research has a a moral imperative to fix the traditional paradigms and ensure that every participant gets access to the best possible care. In this article, we’ll  discuss the evolution of clinical research, how to adapt it to our current needs and life styles, and how to incorporate more hybrid decentralized trials (DCTs) and fully decentralized trials into clinical development. Doing so will better integrate healthcare into participants’ real lives and accelerate approval of new medications.
discuss the evolution of clinical research, how to adapt it to our current needs and life styles, and how to incorporate more hybrid decentralized trials (DCTs) and fully decentralized trials into clinical development. Doing so will better integrate healthcare into participants’ real lives and accelerate approval of new medications.
The Current Clinical Research Paradigm
The industry unwillingness to adopt innovative changes is partly because the traditional model took a long time to  build. Thousands of working processes depend on traditional paradigms. The technology we have today didn’t exist when we built this traditional model. Yet, despite many technological and telecommunications advancements, the healthcare industry is slow to adopt change. For example, it took 25 years for the industry to move from using paper to electronic medical records. The push for a new model is crucial to executing successful and efficient trials.
build. Thousands of working processes depend on traditional paradigms. The technology we have today didn’t exist when we built this traditional model. Yet, despite many technological and telecommunications advancements, the healthcare industry is slow to adopt change. For example, it took 25 years for the industry to move from using paper to electronic medical records. The push for a new model is crucial to executing successful and efficient trials.
The current, traditional business model is not sustainable — it’s incompatible with the positive, disruptive changes that everyday technology enables. The more time and money spent in clinical development, the more participant lives are at risk.
Drawbacks of the Current Model
Since the 1980s, we have made limited changes to how we develop and test new medical products in clinical research. The FDA is in the process of modernizing, but legacy frameworks are sometimes slower than participant needs. The current, traditional system and clinical research protocols require many on-site procedures that take up participants’ time.
The majority of protocols today have an increased number of procedures or visits a participant would receive for their disease management in the normal course of care. As a consequence, this makes the participant burden high, making it difficult to recruit and retain clinical trial participants. Participants must journey to sites  that may be far from their homes — an average travel of two to three hours — when they could instead pick up a prescription at a local pharmacy, participate in telehealth visits, or use in-home healthcare. As a result, only about 3% to 5% of eligible participants get to enroll in clinical research and there is a 20% to 40% dropout rate for those who do enroll across all clinical trials.
that may be far from their homes — an average travel of two to three hours — when they could instead pick up a prescription at a local pharmacy, participate in telehealth visits, or use in-home healthcare. As a result, only about 3% to 5% of eligible participants get to enroll in clinical research and there is a 20% to 40% dropout rate for those who do enroll across all clinical trials.
The vast majority of today’s population are millennials, who use digital technology daily for nearly all forms of activity — they expect healthcare to maneuver the same way. While the healthcare system is taking steps towards integrating technology — for example, telehealth — there has been little movement in the clinical trials space. As a result, participants are less willing to partake in clinical trials that do not utilize some mobile form of technology. Studies show that about 75% of people preferred a DCT over a traditional trial, and 80% of participants are more likely to take part in a trial that uses mobile technology.1
It’s not just recruitment and rentention that is difficult using the traditional model. Studies show that, without technological tools, data is often noncompliant.
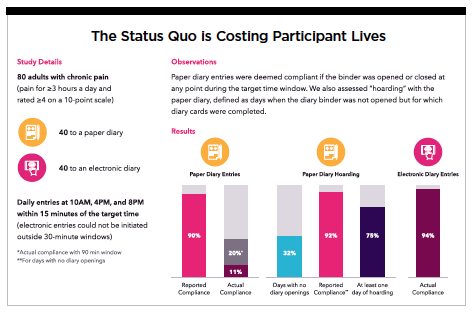
For example, 20% to 30% of patients do not adhere to their medication regimens that are curative or relieve symptoms.2 Between 30% and 40% of participants fail to follow regimens designed to prevent health problems, and 50% of participants fail to adhere to their long-term prescribed medication. The result of these failed drug adherences is billions of dollars to pharma companies. On the other hand, participants were 94% compliant when their diary entries were electronic vs. paper diary entries at 20%.3 (See study graphic on page 27.) Virtual engagement can significantly impact drug adherence and participant behavior, saving time and money that could be better spent on developing treatments that improve patient lives.4
The Need for a New And More Efficient Model
 Given the challenges of our current, traditional model, the industry must be proactive. We must adapt today’s communication and digital health technologies to incorporate into trials, making them more efficient, safe, convenient, and cost-effective.
Given the challenges of our current, traditional model, the industry must be proactive. We must adapt today’s communication and digital health technologies to incorporate into trials, making them more efficient, safe, convenient, and cost-effective.
What Do We Need? There’s a push by participants to use telehealth and digital engagement for their healthcare interaction. The healthcare and clinical research industry needs to incorporate today’s technologies into how we run clinical trials.
How Do We Do This? Create a multi-functional and inter-operable mobile platform that is regulated and allows participants to participate in clinical trials. This platform collects data for a trial in a digital environment in order to be congruent with how participant healthcare is delivered.
What Would it Look Like? It would maxamize participant recruitment with regional, state, or country DCTs, and we’d use hybrid and full DCTs to reduce cost and resources, optimizing efficiencies in all steps. It would also involve a new circle of care, providing access. Through their device, the participant would have access to caregivers, friends and family, CRC/Site, sponsors and CROs, mobile HCPs, and PI/HCPs. We’d implement more mobile participant engagement, using devices anywhere — bring your own device — as personal mobile devices are preferred form of connectivity. Using technology, we can partner with FDA to create new validated endpoints.
What would a new and more efficient model offer? It would offer real-time participant data insights, enrollment insights, de-risk trials in real-time, enhanced participant engagement and safety, participant-centricity and empowerment, and on-demand support.
FDA’s Commitment to Innovation
The FDA has recently demonstrated an open stance towards new ideas and technological innovations. The agency created a regulatory framework supported by key guidance documents. With the issuance of the new Digital Health Innovation Action Plan of 2019, the agency acknowledged that “digital technology has been driving a revolution in healthcare"5 and indicated that use of smart phones, social networks, and internet applications provide innovative ways to monitor health and well-being.
Additionally, in 2020, the FDA created the Center of Excellence for Digital Health Technologies,6 which is dedicated to the advancement of digital health technology, including mobile health devices, Software as a Medical Device (SaMD), wearables when used as a medical device, and technologies used to study medical products.
The FDA-sponsored Clinical Trial Transformation Initiative published recommendations for conducting DCTs through telehealth and mobile healthcare providers. By understanding the convergence of people, information, technology, and connectivity to improve health care and health outcomes, the FDA is more progressive than some sponsors and drug development organizations.
We should take advantage of the FDA’s positioning around mobile health, health information technology, wearable devices, and telehealth to incorporate mobile technology into each new protocol and approach clinical trials from a participant-centric perspective.
Conclusion
Technology is an integral part of modern-day life. Clinical research is evolving by adding digital health technologies and decentralization of operations to enhance convenience to participant engagement while executing more hybrid DCTs and full DCTs. Doing so will reduce the burden on participants who otherwise would be traveling to sites and will reduce billions of dollars in excess costs.
DCTs enabled by technology may also increase recruitment rates, allow for more robust data, quicken the medical product approval process, and — most importantly — save participant lives.
References:
1 https://pubmed.ncbi.nlm.nih.gov/31312746/
2 https://pubmed.ncbi.nlm.nih.gov/17439645/
3https://www.ncbi.nlm.nih.gov/pmc/articles/PMC111114/
4https://www.amjmed.com/article/S0002-9343(16)30844-0/pdf
5 https://www.fda.gov/media/106331/download
6https://www.fda.gov/news-events/press-announcements/fda-launches-digital-health-center-excellence
PRA Health Sciences is developing life-saving and life-improving drugs with our comprehensive clinical development and digital health services. We’re interested in seeing results and getting to work with the latest technologies.
For more information, visit PRAHS.COM/DCT.