 As 2020 draws to a close, we reflect on the changes we have had to make in all facets of our lives due to the pandemic. Some were overdue and some are here to stay. Some were easy to adopt and others we resisted. Change of any sort, positive or negative, is known to be one of life’s great stressors. That’s why sometimes we need help from the right source.
As 2020 draws to a close, we reflect on the changes we have had to make in all facets of our lives due to the pandemic. Some were overdue and some are here to stay. Some were easy to adopt and others we resisted. Change of any sort, positive or negative, is known to be one of life’s great stressors. That’s why sometimes we need help from the right source.
With the onset of COVID-19, we, as an industry, immediately realized we needed to shift to virtual clinical trials. This is one of those changes that may be characterized as both overdue and here to stay. For sponsors and contract research organizations (CROs) it is an area that requires assistance from knowledgeable partners. After all, implementing virtual trial elements is not just about the technology, but also about adapting to new procedures and regulations.
It can be difficult for sponsors and CROs to keep themselves aware of the ever-evolving regulatory guidelines, never mind implementing them in a timely manner, but it is their responsibility. In this article we will shine a light on some of the FDA requirements and guidelines around virtual trials in the COVID-19 era and offer some tips for maintaining compliance.
 Visits: Virtual vs. Clinic vs. Remote
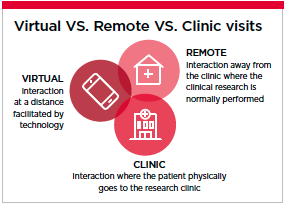
Visits: Virtual vs. Clinic vs. Remote
Before we go on, it is important to define a virtual visit versus a clinic or remote visit. A clinic visit is the traditional interaction where the patient physically goes to the research clinic and has full access to staff, facilities and the instruments needed to conduct the clinical trial assessments. A remote visit is a physical (face to face) interaction at a location away from the primary research clinic. It could be at any alternate location but is most commonly in a patient’s home. A virtual visit is an interaction at a distance facilitated by technology. The people involved are physically separated (not in the same room) and are only able to communicate using telephone, video, internet or some other mode of distance communication.
Virtual Trial Adoption
Prior to the pandemic there was a lot written and spoken about virtual visits. However, according to an industry survey — Virtual Trials and the COVID-19 Pandemic: The State of Clinical Trials — on the impact of COVID-19 on clinical trials, only 33% of companies utilized virtual trial technologies pre-pandemic.
With the demands associated with COVID-19, including government stay-at-home and social distancing mandates, sponsors and CROs who had been merely considering virtualization technologies quickly adopted them as a tool for trial continuation. In fact, the same survey (https://virtualtrials.ert.com) revealed that by as quickly as April 2020 (when the poll was conducted), 82% of participants were already implementing new virtual trial elements.
 FDA Guidance
FDA Guidance
Meanwhile, in March of 2020, the FDA published guidance for the conduct of clinical trials during the COVID-19 public health emergency. The guidance, which has been updated several times, contains specific information on the use of virtual trial technology. Here is a summary of just a few of the points.
Delivering Proper Training
The FDA offers specific guidance about training both patients and site staff on the use of virtual technologies so that patient privacy is protected and data quality maintained. Specifically, study personnel should be properly trained on best practices for video conferencing and telemedicine visits, including how to perform interviews to avoid introducing bias through improper presentation of questions. Patients and site staff should be in a location that prevents inadvertent sharing of any information to others who may be in the area.
Before starting a virtual visit assessment, both the investigator and the patient are required to confirm their respective identities according to a plan developed by the study sponsor. This might include verifying photo identification documents through the video conference, or exchange of photo identification documents through mail or email. The date and time of the virtual visit should be documented, as well as the location of the patient and investigator/site staff.
Maintaining a Reliable Audit Trail
As usual, every step along the way needs to be documented so that sponsors/CROs are audit ready. It’s critical to accurately capture when patients are switched from traditional to virtual trial technologies and what data collection mode is being used for each assessment.
Adjusting Protocols
The modification from traditional to virtual trial technologies will often require changes to the study protocol and procedures. The FDA guidance suggests active communication with all pertinent regulatory authorities, as well as the Institutional Review Board (IRB) overseeing study conduct. Documentation is essential, including information on why a change was made and how the change may impact patient safety and study integrity.
Re-Consenting Patients
The shift to virtual trials may necessitate re-consent of patients. This should be discussed with the IRB overseeing the study. If updated consent is required, the FDA has suggested the use of alternate consent procedures such as electronic consent tools, email or mail exchange of documents and verbal consent with appropriate documentation and witnesses.
Recently, the FDA provided open access to the electronic consent tools available through the FDA MyStudies App as a way to facilitate the informed consent process.
Ensuring Data Integrity
As with any change to a planned investigation, there may be an impact on the statistical analysis of the data. Most notably, missing data and alteration of the data collection methods could introduce additional variability into the study. FDA guidance emphasizes the importance of limiting variability as much as possible when shifting to virtual trial technologies.
The potential impacts associated with any protocol changes should be considered and adjustments made to the statistical analysis plan before final database lock. This may include a comparison of results obtained through virtual technologies compared to traditional data capture methods, investigating differences in compliance by mode of data collection and provisions to adjust for missing data.
If differences are found, data may have to be excluded from evaluation if evidence indicates an impact on the results. In this case, it may be necessary to recruit additional patients and study sites to compensate for the variability caused by either missing data or protocol changes.
Performing Imaging Tests at Remote Facilities
The FDA states that it is acceptable for patients to have medical imaging performed at centers other than the primary investigative site, as long as patient safety and trial integrity is maintained. This will require that the remote imaging site be trained in the imaging protocol for the study, as well as the proper procedures for image acquisition, evaluation, and transmission to the study sponsor.
There are nuances to the regulations that can easily be overlooked. For example, FDA guidance recommends not mixing phone and video communications within a study, but to select a single communication method for use with all patients. Because of these nuances, sponsors need to be deeply immersed in the guidance and also select a technology partner with experts who can guide them through the rapidly changing virtual trial landscape.
Virtual Assessments/Endpoint Collection
Because not all clinical trial assessments can be handled virtually, most virtual trials are usually a hybrid of virtual, remote and clinic visits rather than being fully virtual. That said, we have learned through the pandemic that many assessments and data collection procedures can be successfully converted to a virtual model, so long as they comply with the regulatory guidelines. These include:
Patient Reported Outcomes (PRO): Answers to an electronic questionnaire which is typically given at the research site can be completed either by the patient at home, or by site staff on video conference the phone recording the patient’s responses.
Clinician Reported Outcomes (ClinRO): With proper training, virtual ClinRO assessments can be done successfully provided that the targeted behaviors can be viewed on video, for example when the patient is experiencing pain or tremors or is acting confused.
Performance Outcomes: The FDA recommends that sponsors assess whether evaluation of a performance outcome can be done accurately in a virtual setting. Some assessments, such as range of motion, might be possible through the use of video communication.
Clinical Procedures and Laboratory Tests: Assessments such as blood/urine tests, cardiac tests (ECG/EKG, stress test), lung function tests (spirometry) and medical imaging (radiology) examinations can be done virtually when equipment can be sent directly to the patient and supported by virtual training and data collection.
Managing Risk Through Change
The COVID-19 public health emergency forced a transformation to virtual technologies in clinical trials. But what sponsors/CROs have learned is that once through the implementation curve, there are many benefits to virtual technologies – not just for the duration of the pandemic, but for future clinical trials as well.
However, transformation typically involves risk. Fortunately, the right technology partner can help sponsors/CROs navigate the transformation. By avoiding blind spots, mitigating risk and ensuring compliance with government regulations, they can together open up possibilities for more sustainable, successful trials.(PV)
ERT, a global data and technology company that minimizes risk and uncertainty in clinical trials, so that companies can move ahead quickly — and with confidence, has nearly 50 years of combined clinical, therapeutic, and regulatory experience as well as technology and process‑related insights.
For more informations, visit ert.com.


















