 Many industry leaders believe that one of the most exciting opportunities for improving healthcare is the development of digital health solutions that can help manage disease, improve outcomes for patients and positively support healthcare professionals (HCPs) to improve the provision of care.
Many industry leaders believe that one of the most exciting opportunities for improving healthcare is the development of digital health solutions that can help manage disease, improve outcomes for patients and positively support healthcare professionals (HCPs) to improve the provision of care.
However, in order to be effective, these solutions need to be built on a concept of patient-centered design. This goes much deeper than simply designing a user-friendly interface; solutions that work in the real world must effectively support everyday tasks and the patient’s own goals while also being engaging to use.
Here we review what we’ve learned about designing effective patient support programs and the steps pharma can take to ensure the solutions they provide truly meet patient needs while also aligning with their strategic objectives.
Why Do Patients Disengage?
Let’s start out with some lessons learned. There are so many different ways that digital health programs can provide real patient value, but — not surprisingly — many early digital programs have failed to deliver on their promises. This is because most initial programs were designed to support what the organization (i.e., the pharmaceutical company or healthcare provider) believed would work, or, how they wanted patients to behave.
For example, it wasn’t uncommon for digital health programs to require patients to spend 10 to 20 minutes entering the names and frequency of medications they were taking before providing information of value to them. It’s no wonder patients would rapidly disengage in these interventions.
We now know that patients want control over how they engage with technology; they don’t want to be told how and when to interact, and they expect real value as a result of their interactions. We’ve found that when patients can choose which elements they want to engage with rather than being forced to respond to a cascade of questions, they are a lot more open and willing to continue their interactions with the technology.
 Therefore, we need to provide tools and services that take these and other patient-centric factors into consideration when designing digital health programs. This applies whether the program is intended to improve quality of life, help patients understand their illness, or facilitate better conversations with healthcare providers.
Therefore, we need to provide tools and services that take these and other patient-centric factors into consideration when designing digital health programs. This applies whether the program is intended to improve quality of life, help patients understand their illness, or facilitate better conversations with healthcare providers.
Identify the Value
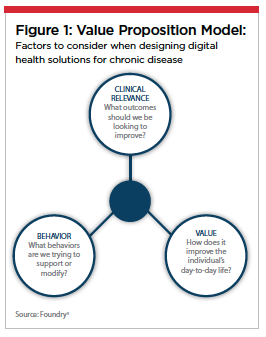
Before jumping into a support program’s design or considering how it can be best executed, it’s critical to truly understand the patients’ problems and explore how a digital health solution might solve them. This can be accomplished through in-depth research conducted with patients, clinicians, academia and health technology experts. These collaborations provide the insight needed to develop a value proposition model that addresses the program’s clinical relevance, behaviors that can be supported and what value the patient will get out of the interaction (Figure 1).
A well thought-out value proposition can serve as the foundation for the design of effective digital health programs that align with the organization’s strategic objectives, rigorously meet real patient need, and are differentiated from currently available solutions.
Clinical relevance
It is essential that digital health solutions address validated needs and produce evidence to measure improvements in clinical outcomes for real people living with any acute or chronic condition. To do this, we must align with significant clinical interventions that work beyond the medicine’s clinical effectiveness. The objective of a support program should be greater than simply focusing on adherence or providing disease information. Solutions need to solve real problems and lead to improved patient experience and quality of life (see sidebar below).
Behavior
The focus for any digital health solution should be on the desired behaviors being sought, not the technology itself. This requires building interventions on a sound foundation of behavioral science. Human beings are not always rational in how they make decisions; this is no different when it comes to health. However, the vast majority of information and services in healthcare are built on the basis that people make only rational decisions. Programs therefore should be created with motivational design at their core to influence improved behaviors.
User value
It is imperative that a solution provides genuine value to the user; this needs to be the primary objective of any digital health strategy. The solution also should integrate with a person’s life and provide support within the context of everyday activities. Anything that makes managing a condition more time consuming or confusing simply won’t be used — as many available websites, tools and applications demonstrate. Although it seems obvious, this focused attention on the user value is not always easy for pharma, HCPs, or academics. Finding the sweet spot of mutual value is the key to success.
Is Technology the Answer?
Our current culture tempts us to throw all kinds of technology into digital health programs, but this approach rarely proves successful. The only way to drive effective patient support programs is by first asking: How can we make patients lives better and create a path forward to engage with them on a longer-term basis? Only then can we make decisions about which technology to use.
When selecting a technology for the purpose of improving clinical outcomes, the key questions to ask are: “How easy is it to use?" and “What are we trying to improve?" Then look for available technologies that address the answers to these questions. So if you’ve identified that patients struggle with getting easily accessible and understandable responses to their questions as they’re managing chronic diseases, then a technology that enables them to easily enter a question and get genuine real-time help might prove to be the most valuable.
An example of this is the use of artificial intelligence (AI) to mimic human conversation and provide a more natural interaction. This technology — seen in commonly used smart speakers like Amazon Echo and Google Home — provides a level of interactivity that apps just can’t deliver.
These voice assistant (VA) technologies provide easily-accessible information when and where patients need it, and offer a significant benefit to patients who are not able to get support through other current technologies, e.g., those living with Alzheimer’s, early onset of dementia and other such diseases. VA technology also opens up doors for providing patient support to elderly patients and others, who, because of manual dexterity limitations are not able to use handheld based-tools (e.g., patients with Parkinson’s disease, Rheumatoid Arthritis, etc.).
The challenge with these tools, however, is for pharma to provide information that is genuinely easy to understand. A lot of content that is currently produced for patients simply doesn’t work when put in the context of an actual conversation, which shows just how unreadable and unhelpful it is from a health literacy point of view.
In Summary: Put the Patient First
Implementing effective patient support programs that work in the real world requires more than technology alone. Programs that will stand the test of time must start with a thorough understanding of patients’ problems before technological tools can do their job and deliver any real value.
The key is to put the patient first. By aligning strategic objectives with patients’ needs and designing personalized programs around individual attitudes and beliefs, digital health solutions can support better, more relevant and highly sustainable patient support programs that truly improve health outcomes.(PV)
ERT is a global data and technology company that minimizes uncertainty and risk in clinical trials so that its customers can move ahead with confidence. With nearly 50 years of clinical and therapeutic experience, ERT balances knowledge of what works with a vision for what’s next, so it can adapt without compromising standards.
For more information, visit ert.com.


















