Regenerative medicine could completely shake up the way diseases are treated. According to Reportlinker, the regenerative medicine market will reach an estimated $50.55 billion by 2025 thanks to the rapid growth of stem cell and gene therapy in developed markets.
 Scott Bruder, M.D., Ph.D., founder and CEO of Bruder Consulting and Venture Group, describes regenerative medicine as therapeutic intervention aimed at the repair, replacement, and restoration of normally functioning tissue that has either been damaged, injured, or diseased through degenerative or traumatic processes.
Scott Bruder, M.D., Ph.D., founder and CEO of Bruder Consulting and Venture Group, describes regenerative medicine as therapeutic intervention aimed at the repair, replacement, and restoration of normally functioning tissue that has either been damaged, injured, or diseased through degenerative or traumatic processes.
Dr. Bruder says the ability to achieve tissue repair depends on a combination of three elements: the cells responsible for synthesizing new tissue; the scaffold material or matrix upon which those endogenous resident cells or exogenously delivered cells exert their influence in the formation of new tissue; and signal molecules, which instruct those cells what to do.
“There are examples of products that are based on one or more of these three ingredients," he says. “For example, a regenerative medicine product may consist of just the matrix, such as a collagen scaffold that looks like a sponge; it could be granules of a ceramic in the setting of orthopedics, or it could be a membrane. In some cases, those sponges or membranes may be pre-seeded with cells, for example, in the setting of cartilage repair or in the setting of bone repair."
There is some skepticism about the use of a single stem cell, growth factor, or scaffold to achieve a complex function. According to Denver Lough, M.D., Ph.D., chairman, president, and CEO of PolarityTE, tissue engineering does not lead to true, fully functional tissue regeneration.
“As we learn more about things we once thought were disposable, such as bacteria, cell waste, and cell destruction, we slowly begin to realize their importance in complex systems, such as the microbiome, metabolomics, and autophagy systems," Dr. Lough says. “It is all part of the interactome that drives integrated complex systems and subsequently the regeneration and neo- generation of tissues. Once we accept this and spend more time evaluating the global processes of tissues and cells, rather than hoping a single gene or drug will regenerate a finger, we will truly begin to develop real, tangible regenerative medicine therapies."
generation of tissues. Once we accept this and spend more time evaluating the global processes of tissues and cells, rather than hoping a single gene or drug will regenerate a finger, we will truly begin to develop real, tangible regenerative medicine therapies."
While Federico Mingozzi, Ph.D., chief scientific officer at Spark Therapeutics, agrees there are still limitations that need to be addressed, regenerative medicine has gone beyond a concept to being a clinical reality in areas such as hemophilia, congenital blindness, spinal muscular atrophy, and forms of primary immunodeficiency.
“With the first generation of gene therapies, issues related to both safety and efficacy were encountered in human trials; most of these limitations seem to have been addressed leading to a renaissance in the field," Dr. Mingozzi says.
Cell Values
There are three different types of stem cells: adult stem cells, embryonic (or pluripotent) stem cells, and induced pluripotent stem cells (iPSCs). Stem cell transplants are either autologous, meaning they are harvested from the patient, or allogenic, meaning they come from a donor.
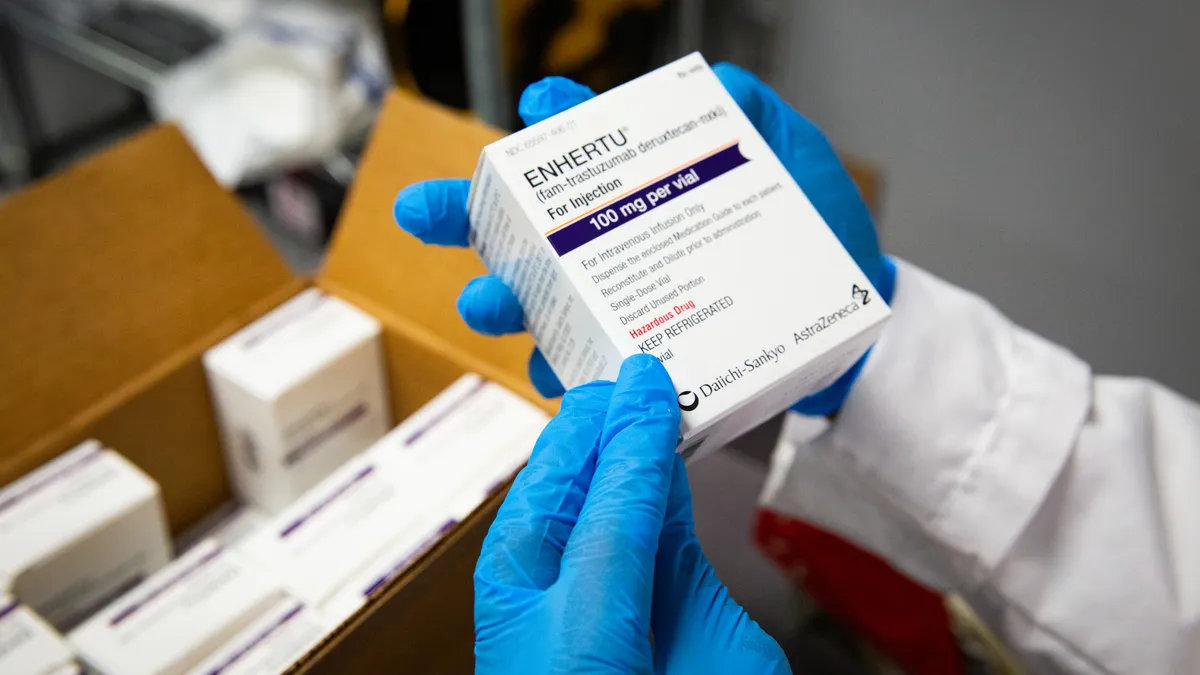
“The use of allogenic cells lends itself more to the pharmaceutical model because companies can create large lots, quality control and cryopreserve them and employ pharmaceutical standards to prepare single dose vials that are ready for delivery," Dr. Bruder says. “This allows companies to substantially increase the scale of manufacturing and subsequently reduce the cost of goods."
Eugene Brandon, Ph.D., senior director of strategic relations and communications at ViaCyte, says the ability to harness the potential of pluripotent stem cells, including embryonic stem cells, has opened countless possibilities. Stem cells are now being differentiated into retinal cells for macular degeneration-related blindness, neural cells for spinal cord injury and ALS, dopaminergic neurons  for Parkinson’s disease, cardiac cells for heart failure, and hematopoietic cells for cancer and transplantation. In the field of diabetes, which is where ViaCyte is working, the focus is on stem-cell derived pancreatic endocrine cells, including insulin-producing beta cells.
for Parkinson’s disease, cardiac cells for heart failure, and hematopoietic cells for cancer and transplantation. In the field of diabetes, which is where ViaCyte is working, the focus is on stem-cell derived pancreatic endocrine cells, including insulin-producing beta cells.
Dr. Lough maintains the unmet promise of regenerative medicine requires a new paradigm, and says PolarityTE is simplifying regeneration, allowing cells to function in a more biologically sound manner with the company’s platform technology to develop a pipeline of functionally polarized, hierarchically organized regenerative tissue products derived from a patient’s own healthy tissue.
He adds that the recent recognition by the scientific field of key and fundamental realities such as the importance and necessity of the interstitium, microbiome, metabolomics and how they orchestrate, design, and command much of the interactome — which drives not just the regeneration of complex tissue systems, but essentially the foundation of life — is bringing the industry closer to significant breakthroughs.
The industry’s scientific understanding has advanced significantly regarding the aging process, the interplay between health and disease, and how stem cells factor in, says Osman Kibar, Ph.D., CEO of Samumed.
 Translating this underlying science into regenerative drugs in the form of stem cell therapies continues to prove challenging from a technical, regulatory, and commercial perspective.
Translating this underlying science into regenerative drugs in the form of stem cell therapies continues to prove challenging from a technical, regulatory, and commercial perspective.
Samumed’s approach has been to target the fundamental molecular processes regarding tissue health.
“We primarily focus on the Wnt signaling Pathway, a developmental pathway that regulates stem cell proliferation and differentiation, and is a key player in restoring and maintaining tissue health, using the innate stem cells embedded throughout our bodies," he says.
Ralph Kern, M.D., chief medical officer and chief operating officer at BrainStorm Cell Therapeutics, says the ability to produce large quantities of high-quality cells through tissue and cell engineering of small harvested cell samples and the ability to cryopreserve the cell products allows for repeated dosing of cell therapies in chronic disease without the need for additional cell harvesting, which greatly reduces the patient burden.
The American Society of Clinical Oncology (ASCO) recognized CAR-T as the 2018 Advance of the Year after demonstration that autologous cell products can be industrialized to create high-value, approvable therapies.
Market Potential
Spark Therapeutics is one of the few gene therapy companies to have an approved product, Luxturna, for patients with an inherited retinal disease that can lead to blindness. The company is developing other therapies based on gene transfer with adeno-associated virus (AAV) vectors for inherited retinal diseases, CNS disorders, and a number of indications for which the liver is targeted with AAV vectors.
“Currently, aside from our work on inherited retinal diseases, we are working on treatments for hemophilia and lysosomal storage diseases," Dr. Mingozzi says. “We’re also working on neurodegenerative diseases."
 One key area of focus for Spark is liver gene therapy. One therapy that targets hemophilia B is being licensed to Pfizer and is entering Phase III trials. Another key program in Spark’s liver platform is a gene therapy for hemophilia A, which is also in the clinic. Preclinical work on Pompe disease is ongoing.
One key area of focus for Spark is liver gene therapy. One therapy that targets hemophilia B is being licensed to Pfizer and is entering Phase III trials. Another key program in Spark’s liver platform is a gene therapy for hemophilia A, which is also in the clinic. Preclinical work on Pompe disease is ongoing.
“While Pompe disease is not a liver disease, we’re exploring this organ as a therapeutic platform," Dr. Mingozzi says. “We used the platform of the liver and AAV transaction of the hepatocytes to perform an enzyme replacement therapy with gene therapy, and we will use the liver as a factory to produce the missing enzyme in Pompe disease."
“We are at the dawn of a new age of biology now and what we are seeing are many cell-based therapies that are not yet approved by the FDA, but are under rigorous clinical evaluation," Dr. Bruder says. “One of those areas that holds the most promise is the management of type 1 diabetes. If we can restore a patient’s insulin-producing beta cells from the pancreas, then we have removed the need for insulin injections two or three, or sometimes more, times per day."
ViaCyte’s cell-replacement therapy for insulin-requiring diabetes aims to be a functional cure by restoring the normal function of a pancreas rather than directly treating the autoimmunity or insulin-resistance associated with type 1 and type 2 diabetes, Dr. Brandon says.
“This could mean that patients with type 1 diabetes will no longer have to be vigilant with blood sugar monitoring and insulin self-administration, as their blood sugar will instead be controlled by the new cells," Dr. Brandon says. “It may also mean these patients have far fewer hospitalizations and may not experience the long-term complications such as heart disease, blindness, nerve damage, kidney damage, and amputations that are so costly to the health insurance system."
Organovo, meanwhile, is using a proprietary 3D bioprinting technology to create a liver tissue “patch" that can be implanted into humans, with the goal of postponing and/or reducing the need for transplant, while also reducing patient care costs.
“Organovo has conducted small animal disease model studies for our lead indication within the category of inborn errors of metabolism, alpha-1 antitrypsin deficiency (A1AT)," says Taylor  Crouch, president and CEO, Organovo. “We have shown that our bioprinted liver patches, when transplanted into diseased animals, have been successfully accepted in terms of generating healthy function and providing notable improvement in liver health."
Crouch, president and CEO, Organovo. “We have shown that our bioprinted liver patches, when transplanted into diseased animals, have been successfully accepted in terms of generating healthy function and providing notable improvement in liver health."
The company was recently granted orphan status for its treatment of A1AT. “The FDA’s action recognizes the importance of novel, tissue engineering-based approaches for these vulnerable patients," Mr. Crouch says. “Organovo’s revolutionary approach to bioprinting functional tissues is opening a broad range of future medical treatments spanning multiple organs and diseases."
Since the discovery of the first Wnt gene in the early 1980s, the Wnt pathway has been a target of great interest for drug development, albeit, with no successful therapeutics to date, Dr. Kibar says. “Our discovery of multiple novel biological targets in the Wnt pathway, our breakthroughs in drug chemistry, and our track record of clinical effort in seven different disease areas, all offer an exciting new path in regenerative medicine, ranging from cartilage regeneration to hair growth, various types of cancer and Alzheimer’s disease."
For example, taking a different approach to addressing an osteoarthritis patient’s pain and functional decline, Samumed’s SM04690 drug is a one-time injection that aims to regenerate the cartilage tissue back to a healthy level, such that the patient can recover his or her active lifestyle.
Increasingly, large pharma companies are looking to regenerative medicine for its potential. In May 2016, GlaxoSmithKline received European marketing approval for Strimvelis, the first ex-vivo — meaning it is prepared outside the body in a laboratory before being administered back to the patient — stem-cell gene therapy to treat patients with adenosine deaminase deficiency (ADA-SCID). Strimvelis (autologous CD34+ cells transduced to express ADA) was the first corrective gene therapy for children to receive regulatory approval anywhere in the world.
Overcoming Barriers
Dr. Bruder says autologous cell therapy has accelerated the application of biologic principles through points-of-care technologies, for example, isolating bone marrow or fat in the operating room for intraoperative manipulation of the cellular sources, which are then delivered back into the patient during the surgical procedure. The challenge with this, he says, is variability that can occur from patient to patient.
“Some unscrupulous firms have made statements or claims about their isolation of these cells, but they are not in compliance with FDA regulations," he says. “Still there are absolutely legitimate companies with FDA-cleared devices for intraoperative isolation of cells used in regenerative medicine."
According to Dr. Lough, patients and providers need pragmatic technologies and therapies, noting that what works in a sterile dish in a laboratory doesn’t mean much.
“Our bodies, processes, and the location where we exist in our environment are incredibly hostile," he says. “Appreciating that our cells, tissues, and processes have evolved over time to survive in these hostile environments requires us to design technologies that are able to tolerate and evolve within this hostility. For example, why would we try to culture intestinal tissue substrates in sterile culture systems — all the intestinal wall does is interface with fecal matter and microorganisms. We must develop tangible and pragmatic technologies that work not only in the trenches of medicine but are also capable of facing the realities that a patient’s own tissue does on a daily basis."
He says PolarityTE was founded by plastic and reconstructive surgeons who saw the realities of the limitations of regenerative medicine and left medical practice to develop something different.
“At PolarityTE we rely on a dramatically different paradigm for regenerative medicine, allowing components in the body to work naturally so that tissues can be used to regenerate themselves," he says.
Dr. Mingozzi says there is evidence that a disease can be treated with a single gene therapy intervention, resulting in long-term efficacy. For example, in hemophilia the follow up of patients receiving gene therapy is up to eight years with no loss of efficacy. However, how long the effect of gene therapy will last and are the long-term effects of these therapies are questions that remain to be answered.
“Recent developments have been demonstrated to be remarkably safe, but at this stage patient numbers are relatively low and as more of these products move into more patients we’ll learn more," he says.
Another barrier, Dr. Bruder says, is the level of investment required. “The manufacturing scale-up for cells or for recombinant proteins typically will require as much as a $100 million investment in capital and facilities, and associated with that is the design, performance, and execution of randomized controlled clinical trials, which will cost anywhere from $15 million to $25 million."
Dr. Brandon says while relatively modest-scale production, testing, and administration is currently feasible, for the groundbreaking regenerative medicines to reach the many patients who may benefit, new scalable manufacturing and delivery systems, including automation and smart systems, will be needed.
Producing enough gene therapy vector to treat disease such as muscular dystrophy or spinal muscular dystrophy with the current technologies is possible, Dr. Mingozzi says, but it is a big undertaking and it’s very costly.
“We will have to find ways to improve the way we execute gene therapies by looking at other more efficient vectors or find better ways to produce these products," he says.
Perhaps the greatest barriers, Dr. Brandon says, are funding for product development, as well as infrastructure and other support for product scale-up.
“Venture and private equity-backed firms are trying to mitigate risk and get to the place where they may have first in-human or ready-to-go into human with a sufficient body of evidence, then put themselves on the auction block to try to get purchased by large companies," Dr. Bruder says. “One example of a recent, large acquisition is Takeda’s purchase of TiGenix."
The time involved is also an issue given the learnings required to translate, develop, and optimize each product, Dr. Brandon says. He cites the California Institute for Regenerative Medicine (CIRM) as an institution set up with a long-term vision.
“With $3 billion to spend over 10 years, CIRM knew to start by building the foundations of infrastructure and knowledge, and that once those were established and underway we would be in a much better position to endure the long and winding product development paths," he says. “In addition, specific patient advocacy foundations, such as JDRF for type 1 diabetes, are committed to providing support to advance therapies that could really move the needle on many diseases."
From a regulatory point of view, the enactment of the 21st Century Cures Act has helped to clarify the pathways related to regenerative medicine technology, Dr. Bruder says. Within the act, regenerative medicine advanced therapy (RMAT) designation can be granted to regenerative therapies that treat, modify, reverse, or cure a serious or life-threatening disease or condition and where preliminary clinical evidence indicates that the drug has the potential to address unmet medical needs.
The next challenge is getting reimbursement, which will require companies to demonstrate the economic health benefit of their products through the generation and availability of data.
The potential for demonstrating economic value is there, experts say. Dr. Brandon notes that the potentially curative treatments that regenerative medicine is expected to bring could provide far greater benefits to healthcare than currently available treatments.
Dr. Kern says the value proposition for regenerative medicine will need to be viewed through a different lens than conventional pharmaceuticals that only modify symptoms, and the required healthcare infrastructure needed to deliver innovative therapies will be an important part of that equation.
As the dialogue to advance these medicines continues, he adds patients, healthcare workers, and families need to be included to identify gaps in the healthcare system.(PV)
~~~~~~~~~~~~~~~~~~~~~~~~~
Regenerative Medicine Advocacy Organization ARM Provides Industry Support
With an objective to advocate for the field of regenerative medicine, the Alliance for Regenerative Medicine (ARM) fosters research, development, investment, and commercialization of transformational treatments and cures for patients worldwide. By leveraging the expertise of its membership, ARM empowers multiple stakeholders to promote legislative, regulatory, and public understanding of, and support for, this expanding field.
Eugene Brandon, Ph.D., senior director of strategic relations and communications at ViaCyte, says ARM provides policy development and promotion, logistical, communications and education, and other support for companies, patient organizations, and other institutions. ARM supports legislation and policies that help the regenerative medicine industry sector develop and thrive.
“In one valuable current initiative, ARM is working with the National Institute for Standards in Testing (NIST) to support development of product standardization, including reference materials and shared quality control assays, that will allow the industry to grow by sharing best practices and common tools between its stakeholders," Dr. Brandon says.
To learn more about ARM, visit alliancerm.org.